Posterior Fossa Syndrome
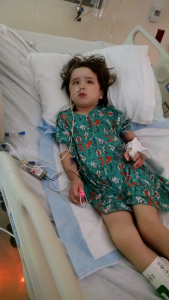
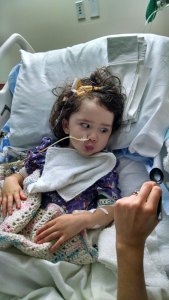
I was not prepared for how Kiara would look after her first major tumor resection. Even though her neurosurgeon discussed the likelihood of her having posterior fossa syndrome, it’s difficult to even type the experience. She was trapped in what can only be described as “neuro storms.” Her mouth and tongue would twitch and her eyes jittered separately and in different directions. She was completely unresponsive to me or any of her caregivers like she was in a coma or far, far away. I knew she was in there and probably scared and hurting, and I didn’t leave her side. I thought she may die at any second because her brain and body were just not right. Her head was strongly tilted to the right and her right eye was completely inward. Her lips were puckered. She had tubes everywhere, including an EVD, two IVs, a feeding tube, and a catheter, plus the pulse monitor and blood pressure cuff. Monitors constantly beeped and alarms went off frequently. It was heartbreaking and devastating.
Posterior Fossa Syndrome is a post-operative condition that affects patients that have had surgery on the back side of the base of the skull that contains the brain stem and cerebellum. Symptoms usually appear 1–5 days after surgery. Most symptoms improve in weeks or months, but some symptoms may continue for years following surgery. The symptoms of posterior fossa syndrome include problems with speech and language, motor skills, and mood changes; however, symptoms can be different for each person.
Over the course of a couple of weeks, Kiara slowly regained control of her face, eyes, and body. Speech therapists helped her relearn how to swallow, eat, and speak; physical therapists helped her regain gross motor skills. There was nothing more terrifying than watching her “neuro storms” after her first major resection, and I was so very grateful that she did not have posterior fossa syndrome after her second craniotomy.